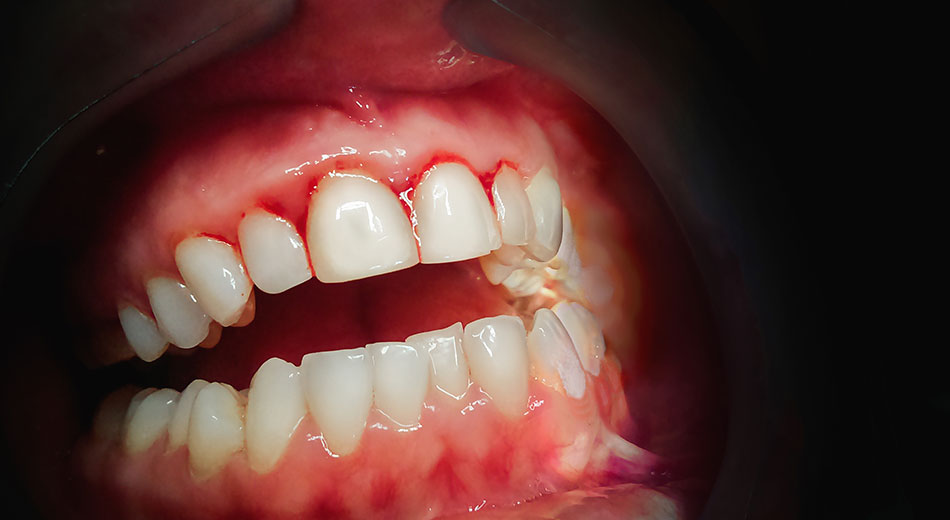
Have you learned that you have periodontitis and don’t know what to do now? Continue reading to learn more about identifying, treating, and reversing periodontitis.
Approximately 50% of the population in the United States is affected by periodontal disease, affecting 65 million people.
We only have one set of teeth throughout our lives, so we must do all we can to preserve them as long as possible. On the other hand, many of us are more concerned with our teeth than with our gums.
We don’t know if our gum health is linked to our tooth health; if our gums are bad, so are our teeth. This results in problems, including loose teeth and root damage.
If you have been diagnosed with periodontitis, it may concern you. The good news is that it is treatable.
Keep reading to learn more about the various types of gum disease and how to treat it so that your mouth is healthier.
Types of Gum Disease
Gingivitis and periodontitis are the two most common types of gum disease.
Gingivitis is an inflammation of the gums. You may be suffering from a bacterial infection if you have it. This occurs as plaque and tartar build-up on your teeth, attracting germs that grow on your teeth and gums.
Poor dental care is the most common cause of gingivitis. It might also be caused by various viruses, germs, molds, and genetics.
Gingivitis is an inflammatory disease of the gums that results from poor oral hygiene. Gingivitis occurs when plaque, a film composed of bacteria and saliva, builds up on your teeth over time.
It will not cause any bone loss or gum recession with gingivitis. Gingivitis is one of the most common forms of gum disease, so it’s crucial to schedule regular checkups with your dentist.
Gingivitis, if not treated, might lead to periodontitis, a more severe condition.
You get periodontitis when plaque and tartar on your teeth are given a feeding ground for germs. If germs are permitted to feed on the plaque and tartar on your teeth, the number of bacteria in the mouth may rapidly grow. Gingivitis becomes periodontitis as a result of this.
Gum disease can cause your gums and teeth to deteriorate. If you don’t act soon, your gums may recede far enough that your teeth will fall out because there isn’t enough gum tissue to support them.
When you have periodontitis, your gums will be inflamed and painful to the touch, and they will also bleed readily. You’ll experience bad breath due to gum inflammation, pus leaking from your gums, unpleasant chewing, and tooth loss. Gum recession may make your teeth in the mirror appear longer than usual.
The three forms of periodontitis are chronic, aggressive, and necrotizing. The majority of people will have one that can be treated.
The most common form of aggressive periodontitis affects children or early adults. This gum disease affects a tiny segment of the population but is devastating. If you don’t act swiftly, you risk bone and tooth loss.
The necrotizing periodontal disease is a severe condition in which gum tissue dies, and an infection develops. People with compromised immune systems are more susceptible to periodontal disease.
Diagnosis
Your dentist may check for periodontitis and its degree based on the following factors: a medical history check to see whether there’re any factors contributing to your symptoms, such as smoking or taking certain prescription drugs that produce dry mouth.
They will rapidly check your teeth for plaque and tartar, as well as bleeding.
The dentist will also insert a dental probe into your mouth beneath your gum line to determine the pocket depth. In a healthy mouth, this gap between the gums and teeth is usually between 1 and 3 mm (mm). Periodontitis indicators include pockets with depths greater than 4 mm. It’s challenging to clean pockets that are deeper than 5 mm.
Dental X-rays look for bone loss in areas with deeper pockets, as detected by your dentist. Your dentist may categorize and grade periodontitis based on the condition of the illness, the complexity of treatment, your risk factors, and your general health.
Treatment
A periodontist, a dentist, or a dental hygienist might assist you with treatment. Periodontitis therapy aims to thoroughly clean the pockets surrounding teeth to prevent tissue damage. You have the highest chance of successful therapy if you follow a daily regimen of appropriate oral care, preserve your health issues that impact dental health, and quit using tobacco.
Nonsurgical treatments
If the periodontitis is less severe, treatment may include less invasive procedures, such as:
Scaling. The dental scaling treatment eliminates tartar and germs from the surfaces of your teeth and your gums. Instruments, a laser, or an ultrasonic device can be used to perform it.
Root planing. The root of the tooth is smoothed during root planing. This eliminates bacterial byproducts that promote gum swelling and delay healing or reattachment of the gum to tooth surfaces.
Antibiotics. Antibiotics may be used topically or ingested to treat oral or periodontal disease. Topical antibiotics include gels and mouth rinses that contain antibiotics in the space between teeth and gums and pockets after deep cleaning. On the other hand, antimicrobial mouth rinses and applications of gel containing antibiotics in the space between teeth and gums and pockets after deep cleaning might be required for oral antibiotic treatment.
Surgical treatments
If you have advanced periodontitis, treatment may require dental surgery, such as:
Flap surgery is a form of periodontal surgery in which the gum tissue surrounding a tooth (pocket) is trimmed to expose the roots for better scaling and root planing. Because gums infected with periodontitis break down bone, your periodontist may realign underlying bone before suturing the gum tissue. It’s easier to clean these regions after you’ve recovered, and they’re more likely to stay healthy.
Soft tissue grafts. The gum line recedes when the gum tissue is destroyed. Some of the injured soft tissue may need to be reinforced. This is usually done by removing a little amount of tissue from the roof of your mouth (palate) or using tissue from another donor source and attaching it to the damaged area. It can help prevent further gum recession, cover exposed roots, and improve the appearance of your teeth.
Bone grafting. This treatment is used to restore the bone surrounding your root after periodontitis destroys it. The graft might be comprised of tiny pieces of your own or manufactured bone. The bone transplant helps prevent tooth loss by supporting your tooth in position. It also provides a basis for new natural-bone development by providing a foundation for new natural-bone growth.
Guided tissue regeneration. This permits new bone to grow where bacteria have destroyed it. Your dentist may use a unique piece of biocompatible fabric to separate existing bone from your tooth in one method. The material prevents unwanted tissue from entering the healing region by preventing unwanted tissue from entering the healing area.
Tissue-stimulating proteins. A third treatment option is to apply a unique gel to a diseased tooth root. This gel, which contains the same proteins found in developing tooth enamel, promotes the development of healthy bone and tissue.
When to see a dentist
If you experience any of the following symptoms, it’s time to seek treatment. They might suggest a need for immediate therapy or further evaluation to rule out additional factors such as mouth cancer or an abscess.